Delayed Cord Clamping is the practice of postponing cutting a newborn’s umbilical cord instead of immediately cutting it during the third stage of labor and is a best practice for moms and babies immediate postpartum.
To some, delayed cord clamping may seem like a “crunchy” thing to do or one of those “birthing fads” but if you think about it, delayed cord clamping was normal protocol long before women could be even considered crunchy. In fact, humans are the only mammals that immediately cut the cord after birth. Dogs, cats, horses, elephants, etc. all seem to have better things to do than to sever the umbilical cord after their baby is born.
Are humans different than all other mammals? Is cutting the newborn’s cord immediately after birth the best for human babies? In this post we will address these issues and hopefully dispel common myths about delayed cord clamping. Let’s get started!

The Truth About Delayed Cord Clamping
“Another thing very injurious to the child, is the tying and cutting of the navel string too soon; which should always be left till the child has not only repeatedly breathed but till all pulsation in the cord ceases. As otherwise the child is much weaker than it ought to be, a portion of the blood being left in the placenta, which ought to have been in the child.”— Erasmus Darwin, Zoonomia, 1801
The main source of information for this article came from the Delayed Cord Clamping Grand Rounds. The OBGYN in the film got most of his information from these two studies:
- Distribution of Blood Between Infant and Placenta After Birth
- The Blood Volume of the Newborn Infant and Placental Transfusion
MYTH Immediate Cord Clamping Does No Harm
Sometimes, when my (hospital birth) doula clients request delayed cord clamping (DCC) they are told by their care providers that there’s nothing wrong with the modern practice of immediate cord clamping (ICC). The truth, however, is that the babies that receive delayed cord clamping have 40% more blood volume compared to babies that received immediate cord clamping. (source)
40% more blood… is a lot of blood.
Basically, babies whose cords are immediately clamped are phlebotomized or bloodletted. It is my belief that if a baby is supposed to have a certain amount of blood after all is said and done, who are we to say no? But let’s dig a little deeper, shall we?
MYTH Babies Are Born with Insufficient Iron Stores
It’s true that many babies are born with insufficient iron stores to get them through the first year of life. This is why formula and rice cereal, for example, are fortified with iron. This is also why many pediatricians push table foods that are iron rich.
But get this, babies that received delayed cord clamping are less likely to be iron deficient. In fact, these lucky babies will have enough iron stores to get them through the first six months of life, at minimum.
What this means is that babies are not intended to be anemic in their first year of life. And it could quite possibly be the practice of immediate cord clamping that has caused this anemia.
For those that don’t know, iron is a big deal in children. Iron helps neurological development. Basically, it helps babies to develop and get smarter, faster! Giving infants the iron they were intended to receive is important for their development.
Delayed cord clamping allows our children to have healthy amounts of iron stores in their bodies that will support them in their first year of life.

MYTH Delayed Cord Clamping Takes Too Long
Many care providers are in a rush to leave once the baby is born. I hate to say it, but they’re really ready to get out of there. To them, their work is done.
I have a hard time envisioning a few doctors in particular patiently waiting for delayed cord clamping to take place. I feel like they would crawl out of their skin. Sitting there and waiting would be too much!
For the care providers that think DCC would take too long… Could you wait just one minute?
Delayed cord clamping causes 40% increase in blood volume, 45% increase in hematocrit, 50% increase in total red cell blood cell volume and 50% of this change happens within the first 60 seconds.
The remainder happens over the following 2-5 minutes.
By waiting only one minute, a baby benefits significantly!
Sure, waiting for 2-5 minutes would be better, but if a care provider is having a hard time coming around to DCC a compromise might be to only wait for one minute.
(reminder: it’s never too late to fire your OB!)
MYTH Stripping or “Milking the Cord” Is the Same as Delayed Cord Clamping
As a placenta encapsulator, I have the fun task of inspecting placentas after birth. I find this to be quite fascinating as I can sometimes tell if certain things like delayed cord clamping, or too much traction on the cord (sometimes causing a hemorrhage) has taken place. I feel like quite the detective!
One time I had a placenta that had only a small amount of blood in it. I thought this was great as it seemed that this new baby received DCC and got all the blood it was supposed to.
Come to find out, this baby did not receive delayed cord clamping but “milking the cord” instead. Instead of waiting for the cord to finish pulsing, what the care provider did was squeeze the cord with their two fingers and slide it up towards the baby.
(Visualize squeezing honey out of a honey stick and this will make more sense.)
Upon further investigation I found out that many care providers in my area were (and are currently) practicing “stripping the cord” instead of DCC. I’m assuming that this is because the care providers are not ok with waiting to clamp the cord so as a compromise they are milking the cord. I’m also assuming that they think these two practices are basically the same thing.
The truth is that milking the cord is NOT the same thing as delayed cord clamping AT ALL. Stripping the cord leaves babies with too high of hematocrit levels (too much red blood cells) aka polycythemia.
Delayed cord clamping for at least 3 minutes, on the other hand, maximizes a baby’s blood volume without experiencing the high hematocrit.
MYTH Delayed Cord Clamping Causes Bloodloss While Baby Is on Mom
One of the arguments I have heard against delayed cord clamping is that if the baby is on mom’s belly with the cord intact, because the baby is higher than the placenta, the baby’s blood will drain down back to the placenta (because of gravity).
The only way this particular doctor would allow delayed cord clamping is if the baby remained below the placenta until the cord was cut.
This is just silly.
The research shows that the baby will receive the same amount of blood if it is 40 cm below the placenta, 10 cm below the placenta or 10 cm above the placenta.
Guess what’s 10 cm above the placenta? Mom’s chest and belly.
The perfect place for baby to be to receive warmth, attention, care and its blood is on mom.
But get this! The blood flow from the baby to the placenta stops at 45 seconds postpartum, but the blood flow from the placenta to the baby continues long after that! So say a baby was higher than 10 cm, it wouldn’t really matter after 45 seconds because blood isn’t flowing out of the baby anymore, just in. Isn’t that amazing?
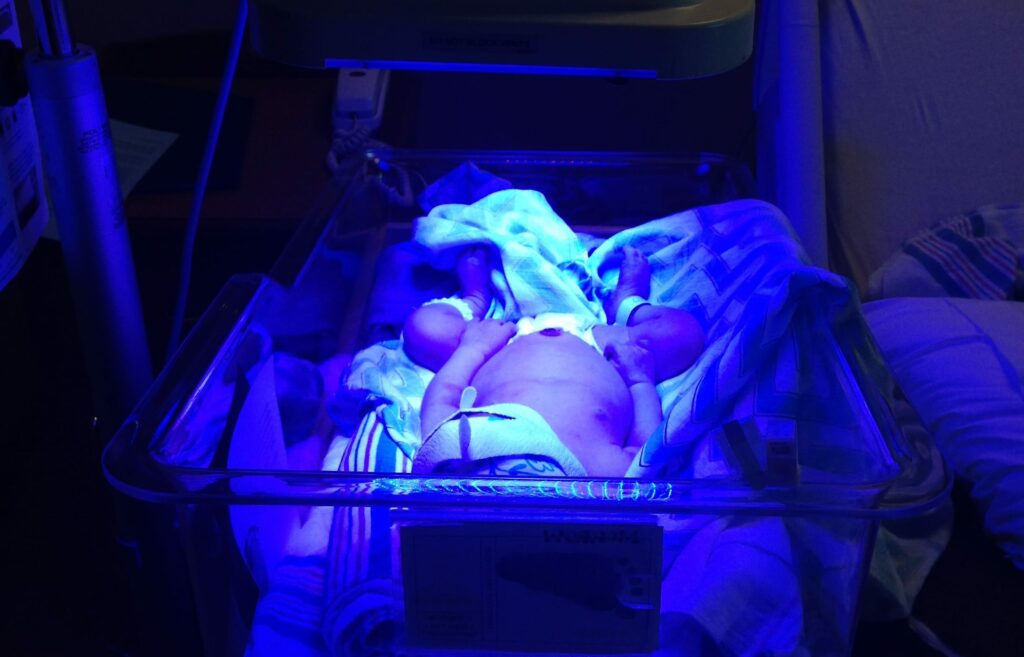
MYTH Delayed Cord Clamping Causes Jaundice
Another argument I’ve heard against DCC is that delayed cord clamping causes jaundice. This is kinda true, but kinda not.
The research shows that DCC does cause higher bilirubin levels, however, these numbers don’t mean much because there was no increase in the number of sick babies.
Delayed cord clamping may cause your baby to have jaundice, but it doesn’t mean that there’s anything wrong.
(I wish more pediatricians were aware of this research because it would prevent a lot of unnecessary jaundice treatments and new parents from freaking out.)
MYTH It Is Better to Immediately Cut the Cord of a Premature Infant
The babies that need all the help they can get are the ones that are born too soon, especially earlier than 33 weeks. At the delivery of a premature baby, typical protocol is to immediately cut the cord and assess the baby in the room on the warmer. Sometimes the baby gets to see mom before she’s whisked off to the NICU, and sometimes not.
Premature babies that received 30-45 seconds of delayed cord clamping had significantly less and less severe in intraventricular hemorrhage (IVH).
(IVH is bleeding into the fluid-filled areas (the ventricles) inside the brain. This condition occurs most often in babies that are born early.)
Also, premature babies are less likely to have sepsis if they receive delayed cord clamping.
A tiny baby that is born too early is a scary thing that no parent wants to face. A tiny baby that is born too early that gets sick is even scarier. By allowing a baby 30, 45 or even 60 seconds of delayed cord clamping their chances of getting sick decrease. I say it’s time to rethink our post-birth protocol and help our babies out.
If resuscitation is an issue, then the technology to resuscitate while still attached to the umbilical cord needs to be created. We got a man to the moon, I think we can do this.
Delayed Cord Clamping
In conclusion delayed cord clamping is awesome! It…
- Allows babies to have full access to the blood they were meant to have
- Decreases anemia in the first year of life helping babies to get smarter faster
- Can be done in a minute (preferably 3-5!)
- Can help premature babies to stay healthy
- Is what nature intended!
According to Academic OBGYN, and the source for this article, “It is not our job to prove that immediate cord clamping is safe. But to prove that immediate cord clamping is not dangerous.”
My Experience with Delayed Cord Clamping
I’ve had a few questions from Mother Rising readers about what my experience with delayed cord clamping was. All three of my births had delayed cord clamping, but my middle child had the most delayed experience of all. 😉

Here I am just after my second baby was born. Do you see that bowl on the bed? That’s the placenta, still attached to my baby. It’s wrapped up in a chux pad.
My amazing midwife took a more casual approach to cutting the cord. She did all the important stuff, like assess me and baby, FIRST. And when she got around to it, maybe an hour or so postpartum, she cut the cord.
And then she examined it, while Eden and I practiced getting a good latch.
And once Eden was is un-tethered, others held her so I could take a shower. And boy, that’s was one of the best showers I’ve ever had!

Talk to Me!
Alright ladies! Leave me a comment and let me know what’s on your mind. Did you have delayed cord clamping? What’s your story? What stood out to you most in this article?


Shelby
Thursday 1st of August 2019
My husband and I are trying to get pregnant right now and I have been reading A LOT about giving birth so that I am more educated to help eleviate some fear and worry. There is so much info out there on what to do and what not to do and I just don't know how anyone can sort through all of it and make a wise decision?! Is there ever a case where DCC would be harmful or dangerous to either mom or baby???
Lindsey
Monday 5th of August 2019
I can't think of one?
Laura
Friday 31st of August 2018
You need to do more research on dangers of extreme levels of jaundice before you post that jaundice poses no danger. Billliruben levels will cloud the brain and cause permanent brain damage. A recent study my doctor told me about since we are pregnant again said 1/3 of dcc helps anemia, 1/3 of dcc shows no benefit or risk and the other 1/3 displayed dangerous extreme jaundice. Guess which category we were in with our daughter before this study came out... we were in the trajectory to hit brain clouding/brain damage high levels without medical intervention and for 3 days we were ferociously pumping, forced to give formula, feeding our child whatever colostrum I could muster up through a finger tube because not for a minute could she come out of the 5 phototherapy lights and for the remaining 2 days in the hospital I got to feed her and spend a timed 45 minutes before sending her back to the lights, then had to bring a billiblanket light home to continue for the weekend and by the grace of god we didn’t have to go to step two which was a blood transfusion. It affectednour bond and I ended up with post pardom, she had the rawest butt Id ever seen because of all the pooping. And because we were trying to/told to have her eat as much as she will take, it really messed with her digestion and enddd up choking at 3 weeks old. She had an insatiable appetite when we found was due to gas as a result of everything and ended up with colic. It was terrible and let me tell you we will not be doing any delayed cord clamping this go-around.
KRISTINE
Sunday 9th of September 2018
Did your daughter get the vitamin K shot? If she did then that will cause jaundice. You are blaming delayed cord clamping( which is completely natural and what God intended) instead of a synthetic Vitamin K shot that has loads of preservatives, including aluminum!!...I think that both together should not be done but that's just my opinion. We did DCC with our son( no shots) and he didnt have jaundice and a friend didn't do DCC and gave vitamin K shot and her son had jaundice so that was enough to convince me that its more then likely the shot causing it not DCC!
Karine la sage-femme
Thursday 24th of May 2018
Than you so much Lindsay for this great and essential article. I use it a lot!!! I an a midwife and teach about quantum approach in birth. I refer to your article in one of my teaching materiel and I have a question: What is the reference to this: "The research shows that the baby will receive the same amount of blood if it is 40 cm below the placenta, 10 cm below the placenta or 10 cm above the placenta." This is a CRUCIAL argument to make doctor changes and I want to feel I have all the references to argue with them! Much LOVE. Karine :)
Jessica Rabbit
Monday 23rd of April 2018
Thank you so much for this article as it has opened my eyes wide on a subject I had already heard about (DCC) but needed more research on. I'm set to deliver this Friday and will definitely plant the seed of DCC into my delivery doctors head.
Candace
Monday 19th of February 2018
Can the hospital make you cut the umbilical cord if you don't want to?
Lindsey
Tuesday 20th of February 2018
A midwife at our local hospital told me she helped fascinate a lotus birth so I guess you have options if you have a good care provider.