Have you ever paused to think about how culture impacts the process of giving birth? Do you ever wonder what giving birth in other countries is like? Have you ever considered that there may be certain practices our culture has adopted less because it’s evidence based but more because it’s “just what we’ve always done”? The following 3 mistakes to avoid immediately after birth are exactly that.

Our culture has a preference towards physician centered care but also has one of the highest rates of maternal mortality compared to other industrialized countries. (SOURCE)
While reading about the mistakes to avoid immediately after birth, you may notice that these practices are not mother and baby centered. Unfortunately, they’re more centered around the convenience of care providers or other observers. Mother and baby centered care, while outside of the box for some, has been proven to increase positive outcomes for mothers and babies and should be the goal for maternity care.
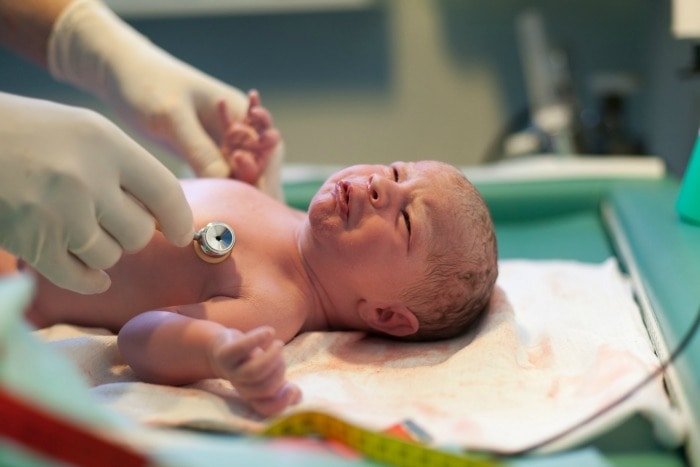
3 Mistakes to Avoid Immediately After Birth
The following mistakes to avoid immediately after birth may feel challenging, especially if it goes against something you have always thought to be true. If you notice yourself resisting a particular idea, I challenge you to ask yourself why. Be curious with your thoughts, and perhaps even bounce them off a trusted friend. 🙂
Let’s get started!
1. Separation of Mother and Baby
“Separation is a 20th century paradigm.” Nils Bergman
First on this list of mistakes to avoid immediately after birth, is the separation of a mama and her baby. When I first became a doula in 2007, cords were immediately cut and babies were taken to an in-room warmer to be assessed, measured, and cleaned before they were allowed to see their mothers. Some babies, however, were lucky and had a couple of minutes of skin-to-skin before they were whisked away.
What I saw years ago was actually an improvement to going even further back, where babies were taken out of the room, and for longer periods of time. Some mothers weren’t even awake for their births! (A former co-worker of mine once told me that after she woke up after giving birth she picked up the phone and asked the nurse if she had a boy or girl. Wrap your mind around that one.) At least these 2007 babies were kept in the same room as mom. Yay?
In recent years there has been a shift in my community encouraging babies to stay with their mothers, and skin-to-skin for the first hour or so after birth. It has been such a joy to see the benefits of this first hand.
Babies should not be separated from their mothers. Just because it’s something we’ve always done, doesn’t mean it’s what we should continue to do. And all the mamas said Amen.

Bathe the Baby
“Glucose levels in infants are higher with skin-to-skin as they don’t spend any energy warming themselves.” – Nils Bergman
When I first began attending births it was standard protocol to bathe babies within the first hour. Let me tell you, these babies were NOT happy about their bath (nor life for that matter). They spent a lot of energy crying but also regulating their temperatures. Wet babies in air-conditioned hospitals get cold fast. By the time these babies got back to their mothers, they were exhausted and breastfeeding became secondary to rest.
Bathing baby soon after birth isn’t typically necessary. Babies aren’t dirty! In fact, it’s just the opposite. Infants have a protective layer of vernix, a white “cold cream” like substance, on their skin that acts as an anti-biotic that NEEDS to stay on. Instead of washing it off, consider rubbing it in. It’s there for a reason! (SOURCE)
Infants aren’t meant to be separated from their mothers and they certainly aren’t meant to spend lots of energy regulating their own temperatures. Delay the bath! It’s not as high of a priority as breastfeeding, bonding, and healthy glucose levels are.
TIP: When mamas are in labor they get really hot. By the time baby is born the room can be quite chilly because mama requested the ac to be set at arctic blast and the ceiling fan to tropical force winds. This environment is great for a laboring mom, but not so great for a fresh newborn. Once baby is born, turn the fans off and the ac to a normal temperature. This will help baby out a lot!

Swaddle the Baby
If for some reason a baby cannot be held by a human being skin-to-skin, sure, the next best thing is for it to be swaddled. Swaddling keeps babies warm but also keeps their startle reflex from… startling themselves. Swaddling keeps babies snug as a bug in a rug.
But don’t be fooled! Swaddling isn’t the gold standard immediately after birth. Babies do best when they’re skin-to-skin with a human, preferably their mother.
If your baby gets handed to you all swaddled up, feel free to unwrap your gift and set that sweet baby on your chest. (You can even do this during a cesarean birth!) Trust me on this, everything is better with a little bit of skin-to-skin. It’s real good stuff.
TIP: Ask for a heated blanket to place over you and your baby. The warmth and the weight of the blanket can help settle post-birth shakes, which are normal, no matter how you give birth. The heated blanket will also help keep your baby warm in a chilly hospital room.
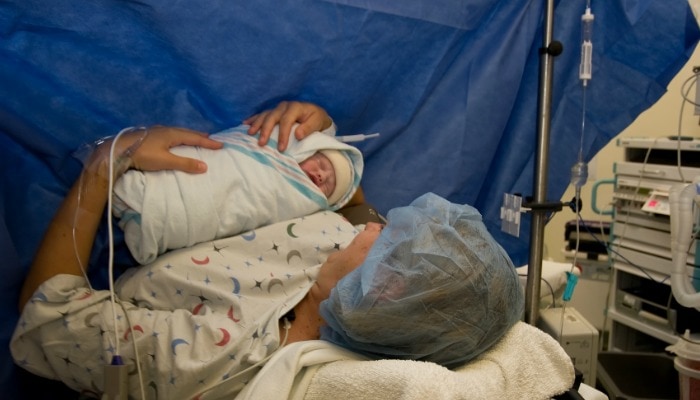
Pass the Baby
“The habitat of the infant is the mother.” Nils Bergman
You guys. One of my biggest pet peeves in this life is how immediate postpartum is handled. One aspect of this that almost sends me through the roof is when parents, family, and friends PASS THEIR FRESHLY BORN BABY AROUND. OH MAN.
As a doula, I rarely hold babies, especially right after they’re born. Even when offered! It’s not because I don’t like holding babies (I actually think it’s the 8th wonder of the world 😉 ) but because it’s not my place. Babies are supposed to be with their mothers. Sure, there are extenuating circumstances where it can’t happen, but as a standard, infants should be with their moms.
TIP: If for whatever reason mama is unable to hold her baby, the next best thing is dad or another family member/friend. Dads, take off your shirts, put your baby on your chest, and cover both of you with a blanket. It may feel a little awkward at first, but you’ll be a pro in no time. You got this!

2. “You Get Pitocin! You Get Pitocin!” – Oprah 😉
New parents are shocked to discover most women that have a hospital birth will receive pitocin right after birth. Pitocin is routinely given to all women to reduce the chance of postpartum hemorrhage. Postpartum hemorrhage is excessive bleeding that occurs within 24 hours after birth and is a major contributor to maternal mortality in low-income countries.
Are parents shocked that care providers want to reduce excessive postpartum bleeding? No. Some expectant parents are shocked because their birth plans specifically state their preference to not use pitocin in labor. They had no idea they needed to address pitocin administration right after birth as well.
Other new parents are shocked because, while they were consumed with meeting their new baby for the first time, they had no idea pitocin was put in their IV.
I think the issue here is not that care providers want to use pitocin to help make birth safe for women, it’s the lack of informed consent and coercion tactics used with women when they are in a vulnerable position.
Sure, maybe you are at a higher risk for postpartum hemorrhage and pitocin may be a wise choice! It just shouldn’t be slipped in a woman’s IV without a conversation. Informed consent is the right thing to do.
TIP: Also, pitcoin is linked to postpartum depression. Have a discussion with your care provider before labor to see if this medical intervention will be the best choice for you.

3. Let it Be (the Cord)
Milking the Cord
Umbilical cord milking is where the cord is pinched and “milked” immediately following birth, or the third stage of labor, in order to quickly push blood into the baby (as you would squeeze ketchup out of a packet, or honey out of a honey stick). Starting as close to the placenta as possible, moving towards the baby, a care provider milks the cord several times before the cord is finally clamped and cut, usually within 20 seconds. Umbilical cord milking is also sometimes called “stripping the cord”.
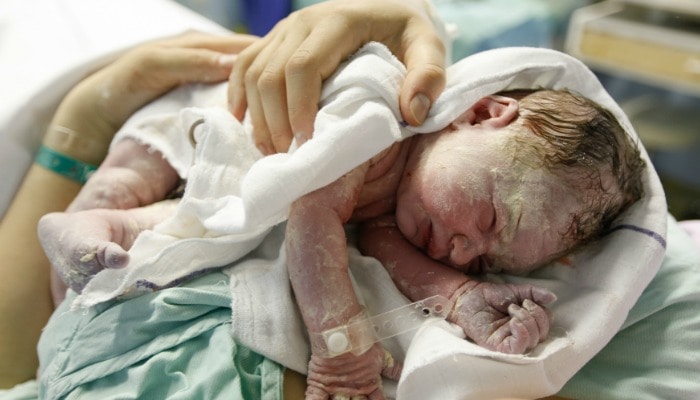
Delayed Cord Clamping
Delayed cord clamping, on the other hand, is the practice of postponing cutting a newborn’s umbilical cord instead of immediately cutting it after birth. This is a hands off approach where nothing is done to the cord for a few minutes, or until it stops pulsing.
In recent years, ACOG and the AAP have both backed the practice of delayed cord clamping at birth for term and preterm infants.
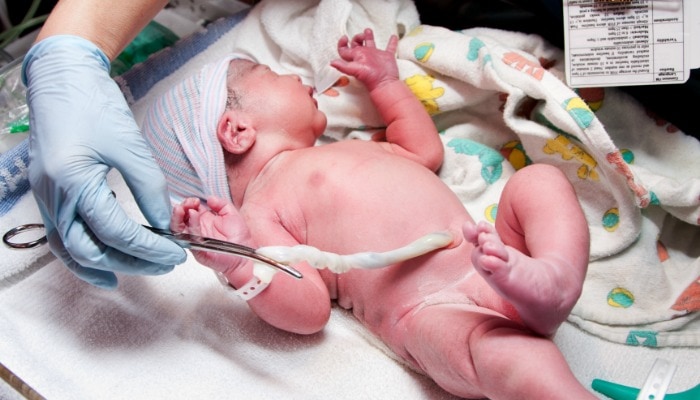
It’s Not a Tube of Toothpaste
However, in my community, and perhaps in yours too, many care providers are now providing umbilical cord milking in lieu of delayed cord clamping. On the surface, it makes complete sense. Why wait minutes for blood to make its way to baby if you can push it through in seconds?
However, as you may have already guessed, delayed cord clamping and umbilical cord milking are not the same. Umbilical cord milking could leave babies with too high of a hematocrit level (too many red blood cells) aka polycythemia. (SOURCE)
Have a conversation with your care provider about delayed cord clamping and see what they think about umbilical cord milking. I bet you’ll have an interesting conversation!

It’s Not a Tug of War
One of my side hustles is placenta encapsulation, where you guessed it, I mess with a lot of placentas. Every now and then I’ll get a placenta that is almost in pieces, and looks pretty mangled. If a doula was present at the birth I will often text and ask if the mama hemorrhaged. Often, I get a yes, followed by a “how did you know that?”.
You see, most care providers use cord tension to help a woman deliver the placenta in one piece and in a timely manner. It’s pretty standard across the board. Other care providers, however, are in a hurry and pull on the cord to make it come faster.
Pulling on the cord may work some of the time, but other times will leave pieces of the placenta inside the mother (this is called retained placenta), which can cause postpartum hemorrhage, and if not eventually expelled could lead to an infection.
In high resource settings (like ‘Merica) one research study said that any sort of cord tension had no significant effect on postpartum hemorrhage. Perhaps this is another one of those things we do “because we’ve always done it this way”? (SOURCE)
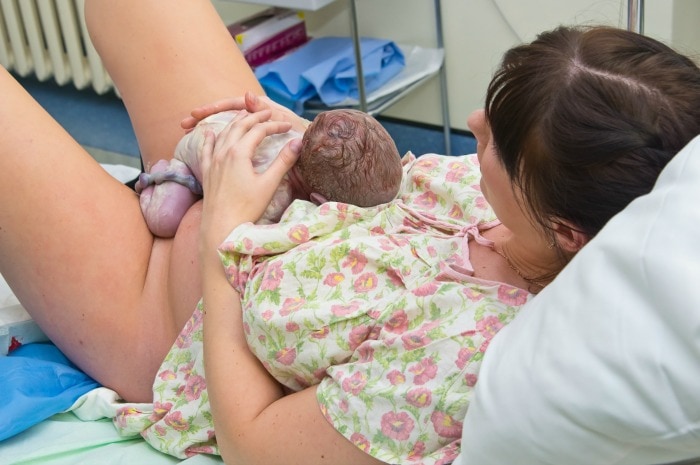
3 Mistakes to Avoid Immediately After Birth
Now that I’ve sufficiently ruffled everyone’s feathers, let’s recap. The following are mistakes to avoid immediately after birth.
1. Nobody Puts Baby in a Corner
Mamas, there’s no reason to be separated from your baby right after birth. Even if your baby needs medical intervention, these procedures can often be done while your baby is still with you. (But that’s another topic for another day.)
*Further Reading
8 Routine Newborn Procedures You Need to Know About
2. “You Get Pitocin! You Get Pitocin!” – Oprah 😉
Have a conversation with your care provider and birthing venue to inquire about their policies regarding pitocin. Do some research to see what you’re comfortable with.
*Further Reading
You Need to Know: Most Get Pitocin Right After Birth
Surprise! Pitocin Is Linked to Postpartum Depression
3. Let it Be (the Cord)
Again, talk with your care provider about how they approach the third stage of labor. If you’re not comfortable with their answer, talk it over with a trusted friend or family member. Maybe they’re not the care provider for you?
*Further Reading
Warning! Umbilical Cord Milking Is Not What You Think
The Truth About Delayed Cord Clamping

Megan
Tuesday 14th of June 2022
It is standard practice for my provider to pull on the cord or use "tension" on the cord. I didn't know this before I gave birth. It never even crossed my mind that they would mess with my body by pulling an organ out without telling me beforehand. I hemorrhaged after the removal of my placenta and the doctor had to put her hand up in my uterus to make sure everything got out. It was traumatizing for me and more painful than birth itself. I feel it is something the doctor should tell you about before doing it. This time I will be telling my doctor to allow for delayed cord clamping and no pulling on my cord, just let me do skin to skin and breastfeed to allow my body to do what it was made to do.
Lindsey VanAlstyne
Thursday 4th of August 2022
Sounds like wisdom to me. <3
Nevena
Friday 3rd of June 2022
So in my country (Serbia)only one hospital do this(skin to skin, delayed cord clamping) for pitocin I'm not really sure. But in other hospital you see baby after hours, they bath babies, and babies aren't with mother during time in hospital. Mothers can see babies only for breastfeeding time. But here most of mamas like that. They want to rest after giving birth. I remember one mother said she is so tired bc her baby cried all the time in hospital and she just wanted to sleep. I'm glad I choose right hospital and my baby and I have all the benefits of spending time together since first second after birth. Yes it can be difficult, but it's beautiful to continue be one with your baby even after birth.
Kllrnc
Thursday 21st of April 2022
As a maternal child nurse, I full heartedly agree. An infant’s place is with Mom then Dad! The nurse should be there to assist, educate and treat problems.
Sabrina
Friday 20th of August 2021
This is great info. I will be getting pitocin as I have a high hemorrhage risk (7th baby, hemorrhage with my 3rd, 4th, and 6th, all girls). Canada seems to prefer skin to skin, no pitocin unless high risk, and never had my cord tugged. They delay cord clamping about a minute. Probably due to my risk immediately following placental delivery. I really hope I don't hemorrhage this time. It scares me, even though my levels after all except my third were good in spite of hemorrhaging.
Hari
Tuesday 20th of July 2021
Great Article! I would like to add/suggest that right after birth have your baby placed on your chest and breastfeed.